Between 2014 and 2016, under the leadership of Katherine Murphy, the Patients Association published three damning reports exposing the poor performance of the Parliamentary and Health Service Ombudsman (PHSO). A summary of those reports can be seen here. Murphy advised patients not to go to the Ombudsman due to the harm caused by their endless delays and woefully inadequate investigations. At that time, the Patients Association would actively assist members of the public through the complex complaint process and their staff would personally attend clinical meetings and tribunals. In 2017, Rachel Power became the CEO and everything changed.
The Patients Association – our purpose.
The Patients Association is an independent patient charity campaigning for improvements in health and social care for patients.
Uniquely for a charity with a remit covering all health and care issues, we work with patients directly: they are our members and supporters, and also the people who benefit from our help and information services. Through our helpline we provide information to thousands of people each year about the health and social care system.
Although the PA states that it works directly with patients, the helpline is used to signpost concerned members of the public to other organisations, which too often signpost elsewhere in an endless game of pinball. Unlike Murphy, Power has no hesitation in advising people to complain to the Parliamentary and Health Service Ombudsman, even though there is currently no active Ombudsman in place and a delay of at least seven months to review NHS complaints.

On 13.5.25, the Patients Association published the following ‘Patient Story’ on their website.
Amina* called us on behalf of her father, who has been in hospital since suffering a stroke last year. Over time, she noticed his eyesight deteriorating and asked hospital staff to refer him for an eye examination. But her request was refused.
When she contacted his GP for help, she was told that referrals for inpatients (people who are currently in hospital) are the hospital’s responsibility, not the GP’s. Confused and frustrated, Amina phoned us to find out who was responsible.
We explained that, according to the British Medical Association, GPs aren’t responsible for patients once they’ve been admitted to hospital: medical decisions and referrals must be managed by the hospital team.
Amina had already raised concerns with the Patient Advice and Liaison Service (PALS), but hadn’t found the response helpful. We talked her through how to escalate the issue to the Parliamentary and Health Service Ombudsman if needed, and also shared details for the Equality Advisory and Support Service in case further support would help.
Thanks to her persistence, Amina is one step closer to getting her father the care he deserves.
(*not her real name)
Amina may be ‘one step closer’, but she still has a marathon ahead of her. Once her seven-month wait is over, she may well fall foul of Rob Behrens’ decision to dismiss cases deemed to be ‘less serious’ to reduce the backlog following the pandemic. This still includes all complaints considered to be at levels 1 and 2.
Level 1 (Minor Injustice): Minimal impact, such as temporary inconvenience or minor distress. Compensation is typically low or may involve non-financial remedies like an apology.
Level 2: Slightly more significant impact, such as prolonged inconvenience or mild emotional distress without lasting effects.
If Amina were fortunate enough to have a full investigation, she would be waiting in a backlog of cases which could not be finalised due to the delay in appointing a new Ombudsman.
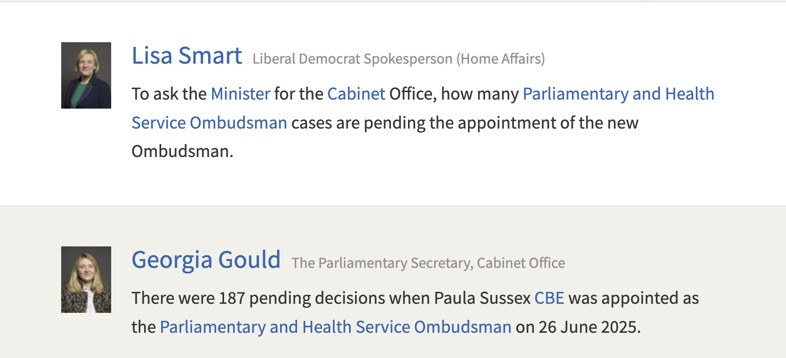
Are the Patients Association completely unaware of the current state of affairs, or perhaps they don’t really care what happens to Amina and her father as long as they can move her off their helpline queue?
Although the Patients Association state that they are “…an independent registered charity that offers support and advice to patients,” they do not raise the majority of their funds from the public. According to the 2022/23 Charity Commission Register (p22), the bulk of their funding comes from ‘Corporate donations/membership’.
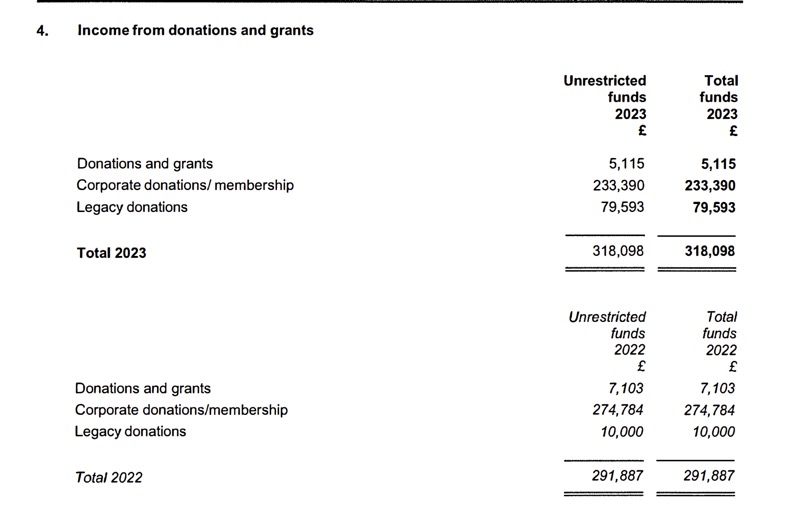
They also earn money from providing their helpline services and from ‘performance-related grants’.

From page 14, it can be seen that the total income for 2023 was £687,689.
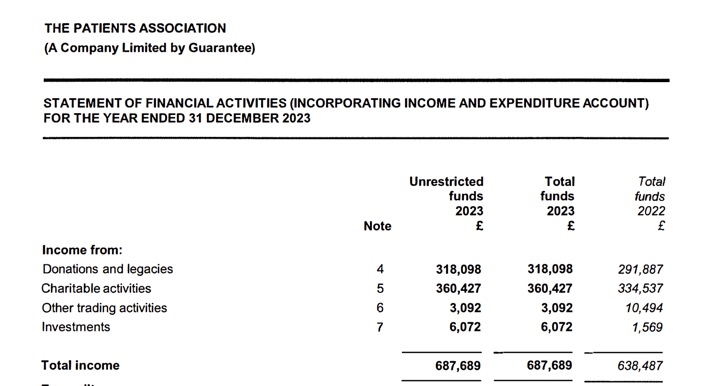
In 2023, this money was used to support a staff of nine who, “…engaged more than 2,000 patients through surveys and focus groups to understand their experiences and inform our policy work. Our helpline supported more than 3,000 callers.” (page 2)
On its Supporters Page The Patients Association informs us that it is independent of government funding to avoid any perception of bias.
The Patients Association does not receive core funding from The Department of Health or any other government body.
Whoever is paying the ‘performance-related grants’ is clearly using criteria to measure the performance of the charity. If this is not the Department of Health or any other government body, then who is it?
The supporters page goes on to list their current ‘corporate partners’ who consist of a range of private health care companies providing drugs, healthcare technology, data anaylsis, legal support, in fact everything required of a modern healthcare system. Take a look for yourself.
To summarise.
The Patients Association is a charity dedicated to supporting patients who have suffered an injustice while receiving the bulk of their funding from the healthcare industry which has been instrumental in causing the harm in the first place.
The Patients Association declined to comment on our concerns regarding their advice for Amina, but then they don’t really answer to people like us, do they.


The Patients Association have shamefully given Amina advice that will ensure that her father does not get the care he needs as his eyesight could deteriorate significantly while she is following this poor advice. Amina should be advised to demand a meeting with the consultant or registrar and insist that she be given the exact reasons as to why this healthcare is being withheld from her father. Record the conversation. It may be that there are valid reasons why the care is being withheld. If not then tell the consultant/registrar that you will consult a negligence lawyer with a view to taking legal action against the hospital. If the consultant/registrar refuses to see you then phone them or write to them again threatening legal action. Record everything. Sadly hospitals tend to ignore patients’ families unless they kick up a fuss. And the PHSO is designed to knock complaints into the long grass. Or even worse to have decisions made against the complainant preventing any further action, legal or otherwise, with the phrase “the Ombudsman has already looked into this and did not uphold the complaint”.
LikeLike
Good advice.
LikeLike
I have to question whether the Patients Association are ‘up to speed’ with the current situation at PHSO regarding investigations. It would appear Amina wanted someone to examine her father’s eyes. To have done so quickly might well prevent the risk of him going blind.
The wider issue is the Patients Association response. I did point out to their CEO how this advice did not look appropriate given there was no recognition of the potential urgency. I received no reply.
The Patients Association has sat on the fence for too many years since completing the excellent work it did under its previous CEO between 2014 and 2016 . PHSO The Facts has, in the not too distant past, tried to bring them back to their original view that PHSO is not fit for purpose. For some reason, they do not want to engage with the issue or us.
LikeLike
Spot on and may i point out that to get to the level of health ombuds in this game of accountability pinball, the NHS service/dept etc must have fully investigated the complaint in writing. So poor Amina, is going to get her complaint rejected by PHSO and her poor old dad, will probaly never get the referral for health care he deserves. But on the bright side, we the oublic, pay the health ombuds (PHSO) around £30 Million a year to play this game. 🥳🤪🥹🥹
LikeLike
Good point. Once Amina gets to the front of the 7 month queue she will simply be told that her complaint is premature and to go back to the trust for resolution.
LikeLike
and by the time the complaint meets the PHSO criteria, it will be out of time (i.e the one year rule) 😚😖😤 #CorruptByDesign
LikeLike
Spot on!
LikeLike